Dear Dosimetrist, First, thank you. Thank you for somehow turning my simulation scans into clinically elegant treatment plans while surviving an inbox full of “quick" questions, last-minute schedule...
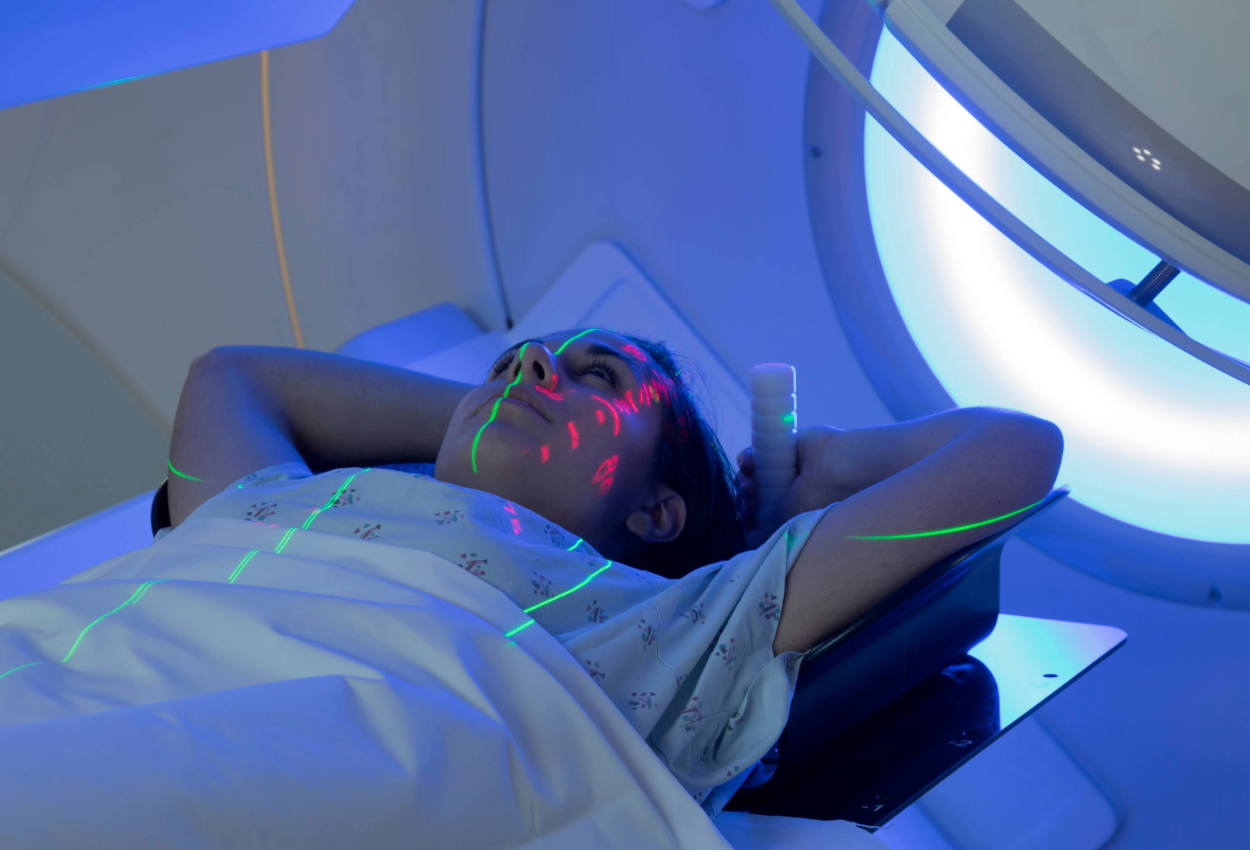
When it comes to radiation therapy set-up marks, one question continues to come up across departments: Should we be using permanent tattoos or temporary marks? The answer has always been: it depends....
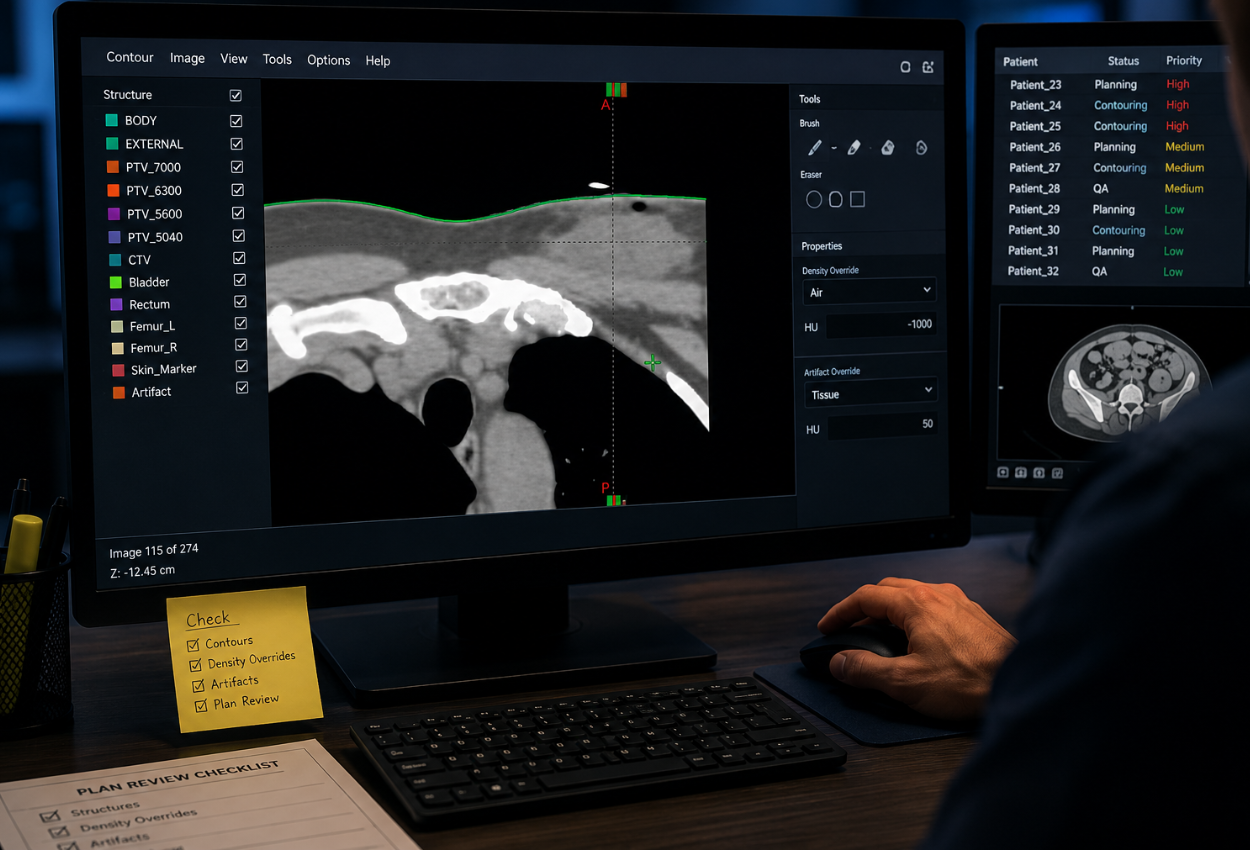
In radiation oncology, medical physicists work hard to protect dose calculation accuracy. Commissioning, algorithm validation, imaging QA, and machine performance are all tightly controlled.But...
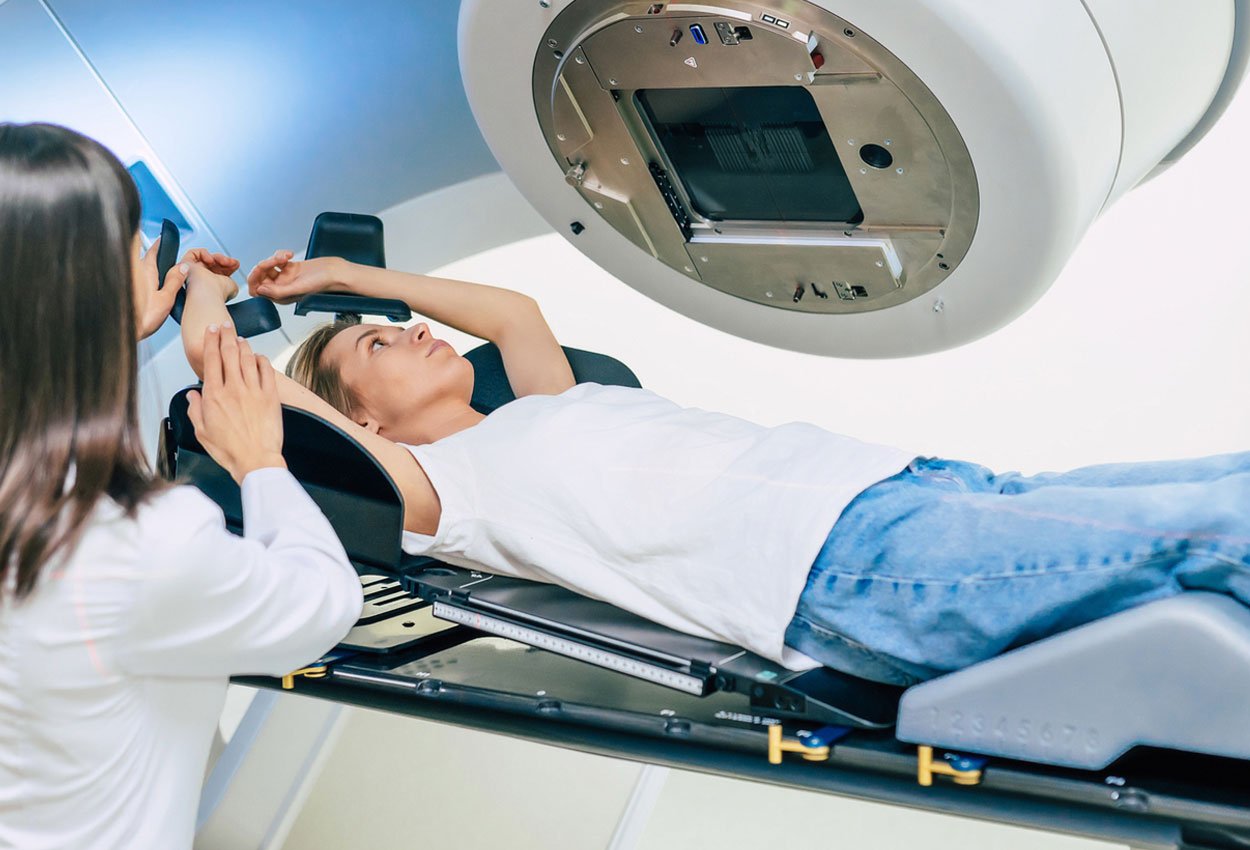
Radiation therapy depends on repeatability. What’s established at simulation needs to show up the same way every day. Most of the time it does but small, human factors can quietly get in the way. One...
As a new year begins, many radiation oncology teams reflect on what is working well and where small refinements could make a meaningful difference. With the continued growth of AI driven planning,...
Hypofractionated radiation therapy continues to expand across oncology, offering shorter treatment courses that maintain clinical effectiveness while improving convenience for patients. As...
Automation has reshaped the body contouring in radiation oncology. Auto-segmentation, atlas libraries, and deep learning tools complete in minutes what once demanded hours of focused attention. The...
To most people, it is just ink. To a radiation therapist, it is a blueprint of care. Every line drawn before that first treatment represents trust between therapist and patient, technology and human...
When patients are told they need radiation therapy, the first question is often, “When can I start?” Every day of waiting feels heavy. And for their care team, every delay feels personal, because...