“We want that body contour to be as accurate as possible. That is what we have to plan through to get to our target – the patient's cancer.” Beth Kelly, Dosimetrist and Chief Therapist, Nash General Hospital, Rocky Mount, NC
Accuracy Is Key In Radiation Therapy
Optimal dose, dose distribution, and the treatment plan make a great difference in the clinical outcomes for the patient. Therefore, it is crucial for the dosimetrist and radiation therapist to clearly define the external body contour during treatment planning.
However, For Obese Patients, Defining External Body Contour Can Be Difficult
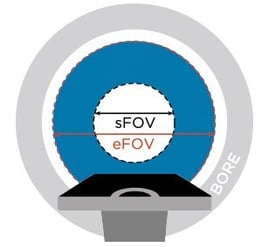
With obese patients, lateral tissues often fall outside the scan field-of-view (sFOV) – usually a 50cm diameter within the CT bore.
Because obesity and weight gain are responsible for nearly 20% of all cancer cases (certain cancers such as liver, kidney, pancreatic, colorectal, and esophageal are more likely to occur in the obese patient) and because this patient population is prone to a greater risk of recurrence, it is that much more important that the treatment plan is as accurate as possible.
 Equipment Allowances For A Heavier Population
Equipment Allowances For A Heavier Population
Many CT simulators do have an extended field-of-view (eFOV) to accommodate larger patients.
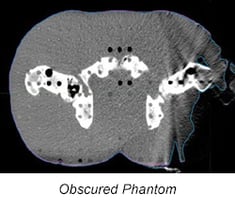
However, artifact is a common obstacle in the eFOV. Noise, beam hardening, and streak artifact degrade the quality of the images. Data can be truncated, skin contour may be missing, and the true density of the tissue lost.
Dosimetrists and therapists are often challenged when dealing with a heavier patient to define a clear body contour in order to accurately measure tumor depth and provide a precise treatment plan.
A Few Common Ways To Compensate For Artifact In The eFOV
1) Treating around the problem by shifting the patient. There are two methods commonly employed that involve shifting the patient on the scanner.
The first method entails the simulation therapist shifting the patient on the table away from the side of interest. The patient is re-imaged but the visualization of one part of the body is sacrificed to image the other. This method limits options for the therapist as it can lead to a loss of data and skin line on the contralateral side, making it difficult to treat through the poorly imaged area.
The second method involves moving the patient to one side of the table and scanning, then moving the patient to the opposite side and scanning again. This can be a labor-intensive effort and exposes the patient to multiple scans which have to be pieced together to create a complete scan.
This, of course, results in an increased dose of radiation. At treatment, greater doses of radiation must be administered to the patient through fewer angles. It translates to a less than ideal treatment plan and more damage to healthy tissue.
2) “Guessing” the body contour. One can define body contour by assigning a tissue density to the missing data and removing the artifact from each of the affected images. Depending on how much tissue is in the eFOV, up to 15% of the image could be affected and have artifact.
Manual removal of artifact can take anywhere from 15 to 60 minutes per patient. More importantly, this method is subject to the interpretation of the dosimetrist. This “guesswork” can put the patient at further risk of receiving an imprecise treatment as some tissue is likely to be over or under-dosed.
According to Ms. Kelly, “When the patient’s body is in the eFOV and you have all that artifact, you’re guessing. I don’t care how much you window and level, you just don’t really know. All I can do is interpolate the data between the posterior and inferior slices that don’t have body contour cut off.”
3) Auto-Contouring Software. Software can reconstruct the images so that an external body contour can be more clearly determined. While this is a preferred method to manual contouring, it is not without its own flaws.
In a 2011 study, the Department of Radiation Medicine at the Roswell Park Cancer Institute found that “image artifacts from eFOV reconstruction alter the CT numbers and body contours of the imaged objects, and has the potential to produce inaccuracies in dose calculations during radiotherapy treatment planning.” Software has improved for the sFOV, but for tissue in the eFOV it remains less reliable
Software alone cannot solve the problem of artifact in the extended field of view, so something more must be done in simulation and treatment planning to clearly delineate the lateral tissues.
Sometimes The Best Solution Is The Simplest One
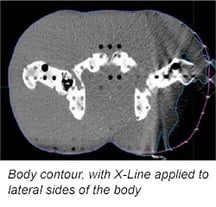
X-Line™ body contour tape for radiotherapy is a radiopaque-lined adhesive tape that is placed along the lateral sides of the patient during simulation to help to delineate the external body contour.
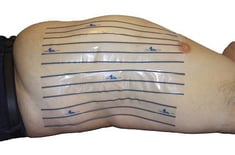
When applied to regions of the body that fall into the eFOV, the three radiopaque lines create hyperdense dots in the CT image slices that make it easy to identify the true body contour by connecting the dots, improving accuracy and saving time for the dosimetrist.
An Actual Body Contour
Beth Kelly was one of the early adopters of X-Line™ and told us, “It gives me an actual body contour. When I apply X-Line to the lateral sides of the body, I have a clean edge to go by. We’re able to ignore and clean out the artifact with software and bring the contour right to that tape on the skin line. It saves me 10-30 minutes and takes out the guesswork. I’ve been doing this for 23 years and it has been a huge help. There’s no doubt in my mind that it makes your contouring more accurate, which any dosimetrist or physician will tell you, is of the utmost importance.”
 Because we believe strongly that accuracy is key and that your diagnosis must be right™, Beekley Medical is pleased to announce that we have partnered with Target Tape, Inc. to distribute X-Line within the United States.
Because we believe strongly that accuracy is key and that your diagnosis must be right™, Beekley Medical is pleased to announce that we have partnered with Target Tape, Inc. to distribute X-Line within the United States.
If you would like to learn more about how X-Line can help you overcome artifact in the extended field of view when treatment planning for obese patients, contact your Radiation Therapy Business Development Manager at 1-800- 233-5539 or email info@beekley.com.
Related articles:

Jonathan McCullough
Product Manager
