
Although we may all see the same thing, how we communicate what we see can vary from individual to individual. While shades of interpretation and unique perspectives can make for great art and interesting stories, when it comes to the detection of cancer in breast imaging - accuracy and consistency in communication are of the utmost importance.
There is a symbiotic balance between the mammography technologist, who acts as the patient’s representative, and the radiologist, who bears the burden of identifying the patient’s images as negative or positive for breast cancer.
Communication between these two individuals must not be subject to interpretation.
A picture is worth a thousand words
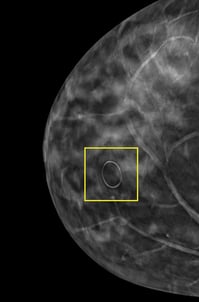 A visual cue directly on an image can be the difference between a cancer being highlighted or ultimately, one being missed.
A visual cue directly on an image can be the difference between a cancer being highlighted or ultimately, one being missed.
With the many aspects of reporting that radiologists must review, a map leading directly to an area of interest or concern can have so much more impact on reading accuracy, as compared to reviewing a separate report with a hand drawing that shows an approximate location.
Seeing radiolucent skin markers directly on the image provides the visual confirmation that radiologists rely on.
Raising the bar to maintain the highest standard of quality
Dr. Amanda Squires , a radiologist with Vista Radiology who reads at Covenant Health in Knoxville TN, is a reviewer with the American College of Radiology (ACR) . In a candid conversation, she shared with us what factors make her job most difficult and the areas she vigorously tries to improve in every aspect of her dual roles.
In her role as an ACR reviewer, Dr. Squires feels that it is essential to raise the bar of expectations to ensure breast centers are maintaining the highest standard of quality - a fundamental principle that she lives by in her own daily practice.
 “In breast imaging, we need to know with precision the relationship of a finding to whatever is being marked on the breast (palpable, surgical scar, skin lesion, point of pain, etc.). Just knowing that two things are in the ballpark range near each other is NOT good enough.
“In breast imaging, we need to know with precision the relationship of a finding to whatever is being marked on the breast (palpable, surgical scar, skin lesion, point of pain, etc.). Just knowing that two things are in the ballpark range near each other is NOT good enough.
“I need to know that it matches exactly on two views and that they move together. If anything is not exactly matching up, more work up is needed. For example, if a patient has a palpable in the upper outer breast and I see fat necrosis in the upper outer breast, I have not definitively explained the palpable area of concern.
“So, mammography skin markers are essential in providing that confirmation. Having a consistent protocol of how the markers are used is a critical component.”
According to Dr. Squires, there is a “significant difference in the quality of work performed in mammography today.”
“When I receive images that fail to give me all the information needed for an accurate diagnosis, I don't get upset about it as I know everyone makes mistakes, but I do have them repeated. I have seen many cases wherein diagnoses would have been different had the image quality been better.
“Quite often, my technologists are even more critical than I am when it comes to images received from outside of our facility. They, too, know it can and should be done better.
Solutions that make communication between technologist and radiologist easier
“Sometimes, doing the same thing over and over can result in a 9-5 attitude.” Dr. Squires acknowledged. “It’s not intentional, but with the increasing demands on their time and appointment windows getting shorter and shorter, it happens. I try to remind everyone that we are saving lives every day and this means everything to the woman entrusting her care to us.
“For this reason, it is so important to me that we offer solutions to our technologists to make their job easier, in any way we can. Consistent use of radiolucent skin markers in both digital and digital breast tomosynthesis is one of those solutions.”
To learn more about the benefits of skin markers for permanent documentation and precise communication in mammography, visit Beekley.com or contact your Beekley Medical Account Specialist at 1-800-233-5539 or email info@beekley.com.
Related articles:

Kathy Kaschuluk
Product Manager
