MQSA’s Enhancing Quality Using the Inspection Program (EQUIP) initiative prepares breast imaging facilities to address image quality on a continual basis and hold the lead interpreting physician and/or interpreting physician as the person ultimately responsible for the image quality. The goal is to ensure that the interpreting physician is continually inspecting image quality and putting corrective actions in place for poor image quality.
Patient Positioning and Imaging Quality
In 2015, the American College of Radiology (ACR) found that positioning is the root cause of accreditation failures - 92% of all clinical images which were deficient on the first attempt at accreditation were deficient in positioning and 79% of all unit accreditation failures for ACR-accredited facilities were due to positioning.
Positioning in mammography is particularly challenging. Mammography technologists have many variables to think through when positioning patients - breast type, anatomy, physical limitations or ailments, as well as their emotional state. No matter how skilled the mammography staff may be, many imaging centers struggle with inconsistencies of positioning techniques and sub-optimal images.
While there is a certain percentage of patients (10-15%) that will result in sub-optimal images because of physical limitations, proper positioning improvements can and should be a focus on all patient images.
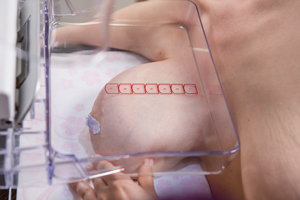 Correct positioning is evaluated on the following criteria: having the nipple centered and in profile, length and shape of pectoralis muscle, pectoral–nipple distance within 1cm in each standard view, visualization of an open inframammary fold, adequate coverage of all breast quadrants and good visualization of the retroglandular space.
Correct positioning is evaluated on the following criteria: having the nipple centered and in profile, length and shape of pectoralis muscle, pectoral–nipple distance within 1cm in each standard view, visualization of an open inframammary fold, adequate coverage of all breast quadrants and good visualization of the retroglandular space.
In their study, "Breast Positioning Mistakes to be Avoided", Popli, Teotia, Narang, and Krishna noted positioning mistakes in 155 of 5382 mammographic views - approximately 3%. That may not seem like a high number until you consider that the study conducted bi-lateral mammograms on 1322 patients and only assessed an equal number of CC and MLO views, 2691 each, and not necessarily matched pairs. The true percentage of positioning errors per patient could be between 5-10%. The most common mistakes found were incorrect nipple positioning, poor visualization of the chest wall, inadequate coverage of lower quadrants, and non-visualization of the inframammary fold.
The authors conclude that breast positioning is the most important factor affecting the mammographic image and that "compromising with even borderline mistakes in positioning increases the likelihood of missing breast cancer and reduces sensitivity of mammography."
So where do you start?
The MQSA EQUIP initiative recognizes that technical image quality issues are not the concern and the focus has been placed on the human factors, specifically compression and positioning.
Bella Blankets® protective coverlets for mammography align with proper positioning initiatives to support EQUIP guidelines and can help with tissue acquisition and other aspects of proper positioning.
You know every millimeter counts when you're looking for clusters of micro-calcifications. Cancers that occur at the chest wall may not be visualized if breast tissue is missing from the image. 80% of Bella Blankets customers surveyed say they get more breast tissue on their images compared to prior images where another product or nothing was used on the receptor plate.1
In a clinical comparison study, 58 patient images using Bella Blankets were compared to prior year images where no protective coverlet had been used to determine if more tissue was acquired with Bella Blankets. The results presented significant improvements that fall under the ACR critical positioning criteria:
- 77% of patients had increased tissue acquisition
- When measuring the PNL in both views, the average increase was 0.41 cm
- 48% of patients showed improved visualization of pectoralis muscle
- Visualization of retroglandular tissue went from 86% PY (prior year) to 96% CY (current year)
- Visualization of IMF as “open” went from 67% PY to 87% CY
Bella Blankets also assist with common positioning issues that technologist face every day such as securing perspiring or oily skin, preventing skin folds on thin or fatty-replaced breasts, holding small/dense breasts under compression, and keeping large breasts "up and out" in the MLO view to ensure an open IMF.
Advancement in Technology to Help Protect Image Quality
 Beekley Medical® is pleased to now offer Bella Blankets with Vertical Channel Technology™ . Vertical Channel Technology (available only from Beekley Medical) allows air to push out and release upon application of Bella Blankets, reducing air bubbles which can cause artifact. In addition, a new easy-lift Pik-UP™ tab allows for clean, easy removal without leaving residue on the receptor plate.
Beekley Medical® is pleased to now offer Bella Blankets with Vertical Channel Technology™ . Vertical Channel Technology (available only from Beekley Medical) allows air to push out and release upon application of Bella Blankets, reducing air bubbles which can cause artifact. In addition, a new easy-lift Pik-UP™ tab allows for clean, easy removal without leaving residue on the receptor plate.
Make Bella Blankets protective coverlets for mammography one of your corrective actions to improve image quality. Connect with your Beekley Medical Account Manager to learn more and to request a complimentary trial evaluation of Bella Blankets with new Vertical Channel Technology.
1 Bella Blankets Clinical Advantages Survey 2017, Beekley Medical®
Related articles:

Melissa Vibberts
Director of Brand Management
