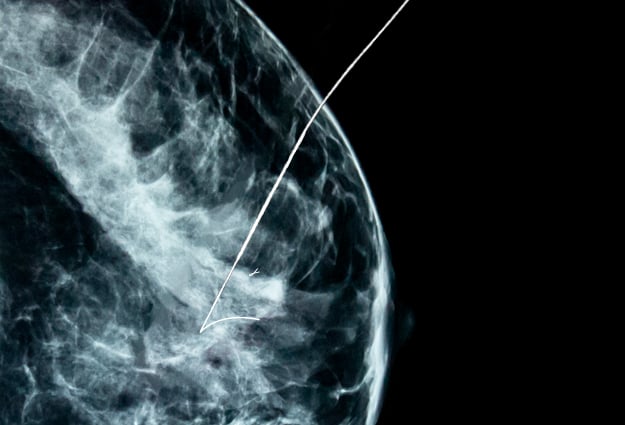
Two recent events reminded us that despite the advances of technology, old challenges remain current challenges in breast health, particularly when it comes to localizing breast lesions for surgical excision.
Both events involved the movement or migration of the guide wires placed under radiographic imaging to identify the area of concern for the surgeon to excise.
A standard of practice for decades
Wire guided localization has been the standard for excising breast lesions for decades, dating back to the mid-to-late '70's. Wire guided localization offered a distinct advantage for both surgeon and patients over the previous method which involved putting the patient under general anesthesia and the removal of large amounts of breast tissue. Seen as a breakthrough technology, wire localization could be performed under local anesthesia prior to surgery and because localization of the lesion was more precise, less tissue needed to be removed for improved cosmetic results for the patient.
Its longevity as the go-to procedure can be attributed to the fact that it is well-established as safe, effective, inexpensive, and as an added advantage - can be employed under mammographic, magnetic resonance, or ultrasound imaging.
However, there are some concerns...
However, wire guided localization does have its disadvantages among which include scheduling coordination on the day of the procedure between radiology and surgery, entry site of the guide wire vs. preferred skin incision site may require larger than desired amount of tissue removal, and the fact that the wire is externally exposed. This external exposure is not only distressing for the patient to see, it also runs the risk of being bent, broken, dislodged, or moved out of place while the patient is waiting for surgery.
One of the concerns with wire movement is that it compromises the accuracy of the localization of the area to be surgically removed.
In the attempt to improve the process or "build a better mousetrap," alternatives to guide wire localization such as radioactive seeding, electromagnetic wave reflectors, and magnetic seeding have been developed and tested as safe and effective, but have their own set of drawbacks and have yet to find widespread use. So for now, guide wire localization remains the industry standard for excisional breast biopsy.
So, how do we protect those wires from moving?
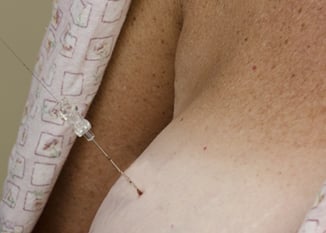
What is not standard is how those exposed guide wires are handled. Practices for covering and protecting the wire vary from site to site and in some cases, doctor to doctor preference within the same facility. Some places opt for no covering, some leave the cannula in for additional support of the wire (which in turn may be protected by taping a cup over the protruding cannula).
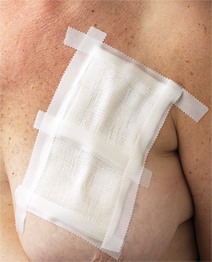 Some cover the wire with gauze and tape it down on the patient's breast. You would this would be make for the best option, but it does have one glaring drawback - the surgical staff needs to remove the gauze before surgery and it is here, where there is no visibility of the wire, that the act of dressing removal can accidentally tug on and/or dislodge the wire from the area it is localizing.
Some cover the wire with gauze and tape it down on the patient's breast. You would this would be make for the best option, but it does have one glaring drawback - the surgical staff needs to remove the gauze before surgery and it is here, where there is no visibility of the wire, that the act of dressing removal can accidentally tug on and/or dislodge the wire from the area it is localizing.
A "clear" solution to stabilize guide wires
After years of struggling with tape, gauze, and cups, a mammography technologist brought her idea for a better way to secure needle localization wires until removal in the OR to Beekley Medical. Cradles® needle localization wire protectors, introduced in the fall of 2008, offered a clear alternative to other methods for protecting the guide wire...literally.
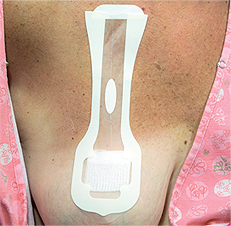 The first professional product created to overcome the challenge of accidental guide wire migration, Cradles are clear covers with self-adhesive edges that stabilize and protect the guide wire while the patient is waiting for surgery without hiding it from view.
The first professional product created to overcome the challenge of accidental guide wire migration, Cradles are clear covers with self-adhesive edges that stabilize and protect the guide wire while the patient is waiting for surgery without hiding it from view.
With the localization wire visible at all times and no adhesion directly over the guide wire, Cradles eliminates the guesswork from the surgical staff and reduces the potential for tugging the wire out of place when removing the wire cover in preparation for surgery.
Established, safe, effective
Cradles has been helping our customers overcome challenges with wire migration in breast localization procedures since 2008.
Contact your Beekley Medical Account Manager at 1-800-233-339 or email info@beekley.com to learn more or to inquire about a trial evaluation of Cradles.
Related articles:

Mary Lang
Director of Marketing Communications